Persistent or Chronic Pain is a very common symptom in people with FND. It is important to recognise that if you do have chronic pain as part of your illness, the two things are probably related.
We have learnt a lot about the mechanisms of chronic pain in the last 10-20 years. Chronic (long-lasting) pain is different to the type of acute (sudden) pain that you get if you cut your finger. It has different mechanisms in the body.
Persistent pain is commonly due to an increase in the ‘volume knob’ in the pain pathways in the nervous system – both the brain and spinal cord. When pain comes from the brain like this is also called chronic primary pain, and also nociplastic plain (pronounced NO-SEE-PLASTIC pain). Common types of nociplastic pain include Fibromyalgia, most people with chronic back and neck pain, and many others.
Persistent/Chronic Pain – also called Nociplastic Pain is a medical condition in its own right
People with chronic pain suffering chronic pain can’t just ‘turn the volume knob down’. The pain is ACTUALLY happening, and at a level in the nervous system out of immediate control.

Chronic (nociplastic) pain can also be seen as a problem, like FND, to do with the functioning of the nervous system which is more to do with the ‘software’ of the nervous system, than the “hardware”.
Here are some videos which help to explain.
The film below is a great short film about women with fibromyalgia from the BBC in the UK. My only gripes…it can be reversible and I don’t agree that it’s unexplained. We have learnt a lot about how fibromyalgia works in recent years.
The commonest types of pain in people with functional neurological symptoms are:
Read more about this problem on this website.
These links also explain more of pain.
Fibromyalgia Information booklet:

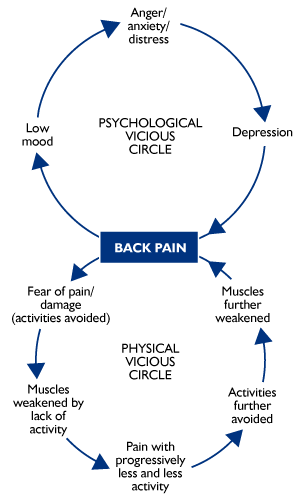
Another thing that management of chronic pain has in common with the management of some functional symptoms is the way in which vicious cycles can develop making the problem worse. For example, if you fall down and hurt your back, you may find for a day or two that its difficult to move because your back is sore. After that time though, moving around slowly increasing your mobility may be the best thing to do. It will be sore, but the more you do it, the less sore it will be.
What sometimes goes wrong, especially after a minor injury, is that people worry that the pain they are experiencing in their back is a sign of something seriously damaged or ‘torn’. Understandably, with this in mind, they may be reluctant to move and may interpret pain as evidence that there is damage and that they should move as little as possible. Eventually however, this approach leads to more and more immobility and more and more pain. The figure opposite illustrates this.
If your main problem is pain you may get further help from a Pain Clinic or a Pain Management Programme which can spend much longer helping you understand your pain better and learn to adapt to it better.
I especially want to highlight the great work being done by Flippin Pain, a public health campaign designed to help people with persistent pain understand and be empowered to improvement. Its contents are free.

I particularly recommend the Flippin Pain formula which highlights the following really important messages
For most people with chronic pain, its hard to improve, even when you understand it. This is because its hard to change your own nervous system. But many people can find ways to make chronic pain more in the background and some people find ways to make pain go away completely. Its hard to make progress unless you have some hope that pain CAN improve, the volume knob CAN turn down.
Living Proof – living proof.org.uk – is an organisation designed to give people with chronic pain and fatigue some hope of improvement. Charli’s video below takes you through her experiences with chronic pain that she had for 2 years before improving.
Fiona had ME/Chronic Fatigue with pain for 14 years but has now made a good recovery. Her video is here
Fiona has published a really helpful 5 Top Tips for dealing with Chronic Pain. Ive listed them below and you can read more at this link.
1. Understand that the brain creates pain to alert us to danger, but that pain is just the brain’s opinion. The brain sometimes gets things wrong
2. Learning to feel safe can calm pain down
3. Social connection promotes healing
4. Understanding your emotions can help reduce your pain
5. Repetition is key


We will be re-directing you to the University of Edinburgh’s donate page, which enable donations in a secure manner on our behalf. We use donations for keeping the site running and further FND research.
